The Inevitable Legal Deconstruction of Gynecological Morcellation Is Well Underway
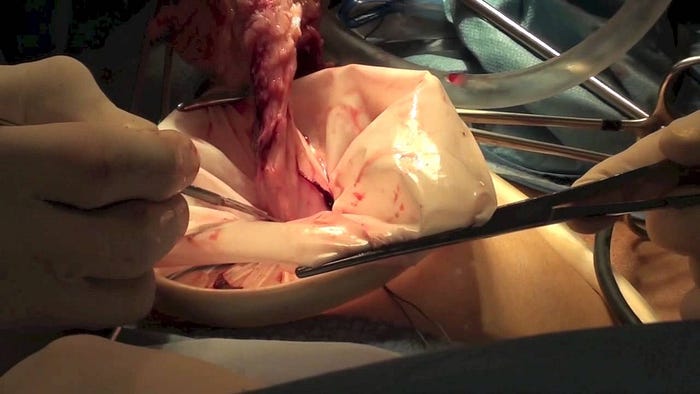
A few weeks ago I wrote an article calling on all medical malpractice attorneys and trial advocates to focus their attention on the negligent practice of morcellation by gynecologists. You can read this article, here.
The fact I presented to plaintiff’s attorneys is that the power morcellator device and the practice of morcellation in Gynecology evolved from an original error—an assumption that proves deadly to a subset of women with occult or missed cancers of the uterus.
This incorrect operating assumption is that uterine fibroid tumors are benign — and that the minority fraction which are malignant represent a small enough subset of the whole to be negligible when considering surgical management of fibroids. Based on this deeply rooted and incorrect assumption in the field of gynecology, morcellation evolved in the gynecological specialty and was accepted as a standard approach for removal of these large tumors of the uterus. Because without accepting this incorrect assumption, no reasonable surgeon could ever accept the catastrophic risk of spreading and upstaging a woman’s cancer using morcellation.
Of course, with the parallel development of minimally invasive and laparoscopic technologies, morcellation was also mechanized and ultimately, the power morcellator evolved to allow convenient and standardized morcellation of large tumors of the uterus. It was an almost forgotten fact for gynecologists that an undiagnosable subset of these tumors are in fact cancerous — and most gynecologists, even to date, are comfortable with the utilitarian argument that morcellation “benefits the majority” and is, thus, justified. But, of course, this line of thinking violates the bedrock principles of medical ethics and a core surgical principle — in particular when a woman’s occult or missed uterine cancer is spread and upstaged by morcellation.
All this changed in November 2013 when the Wall Street Journal reported on Dr. Amy Reed’s complication with a power morcellator at the Brigham and Women’s Hospital in Boston. A large scale public health battle ensued that has led to the virtual demise of power morcellators. A large number of product liability and medical malpractice cases have brought the use of this product to near termination in the United States. Though many women remain susceptible to reckless GYNs who insist on using this device, because companies like STORZ negligently refuse to withdraw their dangerous product from the market, as J&J did.
What’s even more astonishing is that almost the entire field of gynecology is “brain washed” into believing their incorrect assumption about uterine fibroids with near religious fervor — when it comes to their defense of morcellation. The demise of power morcellators, and the serious discourse and battle surrounding it, have not deterred most gynecologists from manually morcellating these tumors in women. These minimally invasive gynecologists have simply reverted to manually morcellating uterine tissues in order to remove the tumors using small incisions. These doctors truly believe that morcellation of potentially malignant tissues and tumors has a place in the treatment of women — and that their small incisions are worth the hazard they are exposing those with occult and missed cancers to. These surgeons are comfortably willing to neglect the risk of cancer spread and upstaging as being an “unfortunate” or “negligible” “trade-off” in their profession. They behave as though Dr. Amy Reed’s public health campaign and the FDA’s action was nothing but an effective “publicity campaign”. So they’ve gone as far as to engage in a reckless “counter-publicity” campaign of their own. But this attempt is both dangerously pedestrian and demonstrative of the depth of unethical thinking and surgical under-education.
Of course, no other surgeons worth their salt buy this disturbed reasoning — because morcellation of tissues with malignant potential is simply a violation of a core surgical principle. And this is precisely why morcellation is, in fact, a negligent standard of care in gynecology.
So, the key to successful litigation of morcellation cases will be for legal teams to demonstrate that though the GYN specialty, accepts this practice as a “standard”, no other reasonable and well-trained surgeons view it as an ethical and oncologically safe practice. In addition, it is a near certainty that expert bioethicists will find this practice to be a violation of the ethical standards of conduct expected of physicians — that element will soon be introduced in courtrooms too, as it was at the FDA hearing of July 2014. Therefore, the very characterization of morcellation as a standard of care by general and oncological surgeons, and by bioethicists, must be interrogated in court.
So it was that at the end of July 2017, nearly two months after my wife’s passing, I penned my message to medical malpractice lawyers and trial advocates calling on them to litigate all cases of manual morcellation where a woman is subsequently diagnosed with cancer. Because every morcellated women with a cancer diagnosis has been put in deadly harm’s way by the operating gyencologist — and there will be many.
I project that the liability incurred by the GYNs and medical centers participating in the practice of morcellation will be large, if malpractice lawyers around the nation do their jobs they are trained to do well— simply because a vast majority of minimally invasive gynecologists are still operating on their incorrect assumption that uterine fibroids are benign and are engaged in this negligent gynecological “standard of care” known as morcellation.

On the heels of my message to malpractice lawyers, I was contacted by attorney Gregory E. Barrett of Illinois informing me that he has filed the first “manual morcellation” case in a US federal district court (IN THE NORTHERN DISTRICT OF ILLINOIS WESTERN DIVISION — Civil Case No: 17-cv 50206).
This case is representing the interests of Ms. Alivia Greenfield of IL, who was a victim of manual morcellation of an occult sarcoma. The complaint alleges that Ms. Greenfield’s uterine cancer was spread throughout her abdominal cavity by manual morcellation of her uterine tumor, negligently assumed benign by her gynecologist. My conversations with Ms. Greenfield over the past year about her diagnosis and clinical course, indicate that this allegation is likely to bear out when subjected to expert analysis and interrogated in court.
I believe that this FIRST case will be one of a flurry of such cases across the nation filed against GYNs, any physicians who enable these operations (i.e., Anesthesiologists), and the medical centers in which these manual morcellations are taking place.
Surely, our system of justice in medical malpractice law has the capacity to recognize when one medical specialty’s “standard” of practice is catastrophically negligent, and is recognized a such by other medical specialists and bioethics professionals observing it from outside the guild.
Morcellation in gynecology is synonymous with medical malpractice and negligence. And, I believe, that a few good plaintiff’s attorneys will make medical history soon — despite the insistence of some very well-decorated gynecologists and industry advocacy groups, with professional and financial interests invested in this dangerous practice on women, that it is safe.
I am confident that, paradoxically and sadly, it will be malpractice attorneys who will deliver the GYN specialty from its self-destructive pattern of professional behavior. Because when it comes to the surgical management of women’s uterine fibroids nothing but the utmost care and universal oncological safety precautions is acceptable - very certainly NOT morcellation based on an incorrect assumption.
In the name of Amy Josephine Reed MD, PhD — Georgina of Yardley.
